Patient Resources
Get Healthy!
IVF 'Add On' Procedure Doesn't Work, Evidence Review Concludes
- April 23, 2026
- Dennis Thompson HealthDay Reporter
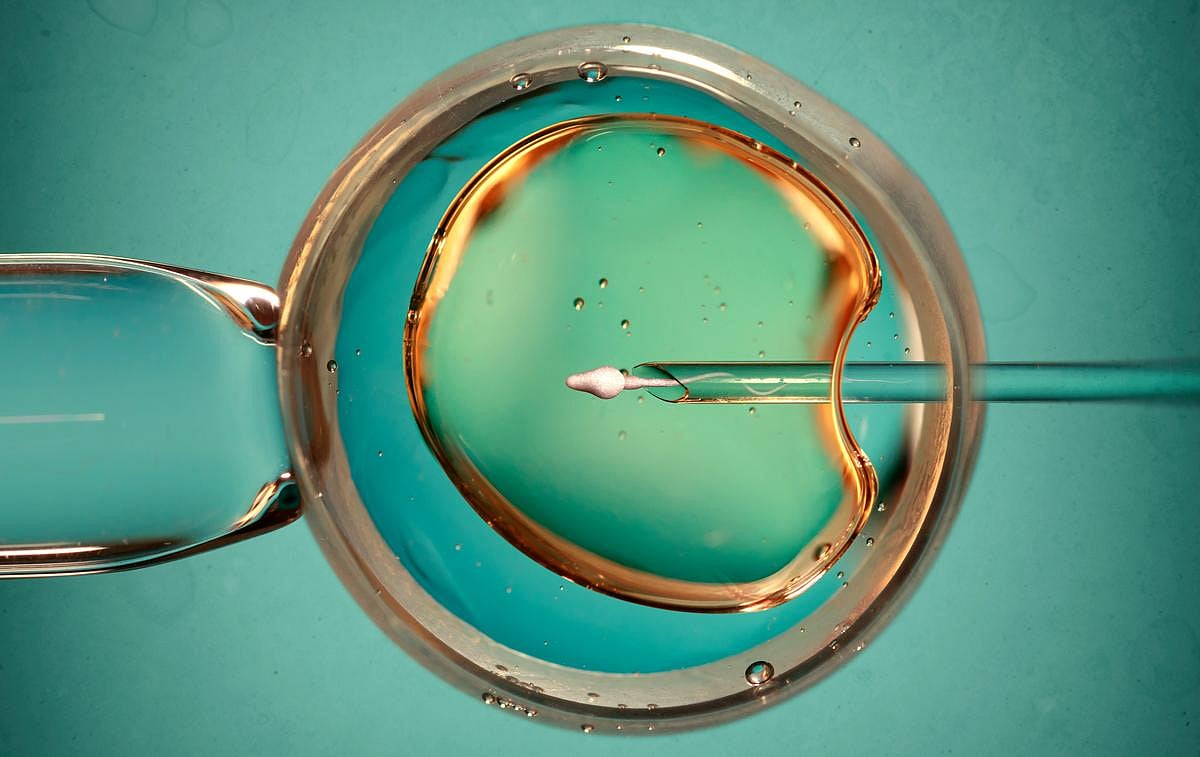
A hormone therapy commonly offered to IVF patients to improve chances of pregnancy is really a waste of time, a new evidence review says.
Injecting the hormone human chorionic gonadotropin (hCG) into a woman’s uterus before embryo transfer does not increase rates of either pregnancy or live births, researchers recently reported in the journal Human Reproduction Update.
“For patients and clinicians, the message is clear: This add-on does not improve fertility outcomes,” lead researcher Rui Wang, a senior research fellow at the University of Sydney in Australia, said in a news release.
“This hormone shouldn’t be routinely offered as part of IVF treatment,” he said.
This hormone procedure is used around the world, including in the U.S., Europe, Australia and parts of Asia, researchers said in background notes.
The procedure became popular in the early to mid-2010s to improve implantation during IVF, based on studies that reported positive results, researchers said.
However, when they analyzed the raw data behind those studies, they found that earlier claims about the positive effects of the hormone therapy didn’t stack up.
For the new review, researchers pooled data from seven previous trials of the treatment involving 2,244 IVF patients. The team looked at the results for the patients themselves, rather than the results published for each individual clinical trial.
Results showed that, regardless of patient type, the hormone procedure did not increase pregnancy or live birth rates.
“There was no evidence of benefit in any group we analyzed, including fresh or frozen transfers, different embryo stages or different doses,” Wang said.
“When we restricted the analysis to studies where the raw data could be reviewed and verified, the effect disappeared completely,” he added.
The procedure is relatively inexpensive compared to the overall cost of IVF, but even though it’s cheap patients shouldn’t be offered a therapy that doesn’t work, Wang said.
“Every procedure offered to patients should be backed by reliable evidence,” he said. “When patients are already going through multiple IVF cycles, adding procedures with no proven benefit is an unnecessary burden on people navigating an already difficult journey.”
Many patients choose these add-ons if there’s even a small improvement in their chances, because they’re often under significant emotional pressure, Wang said.
These findings might be the tip of the iceberg, Wang said. Other add-on treatments in reproductive medicine might have been adopted into practice based on unreliable evidence.
“Many IVF add-ons look promising on paper because early studies report benefits,” Wang said. “But if those studies are flawed or the data can’t be verified, patients may be making decisions based on evidence that doesn’t hold up.”
More information
The Mayo Clinic has more on chorionic gonadotropin.
SOURCE: University of Sydney, news release, April 20, 2026

